Alexia Duveau
Implication of neuronal versus glial purinergic receptor P2X4 in chronic neuropathic and inflammatory pain
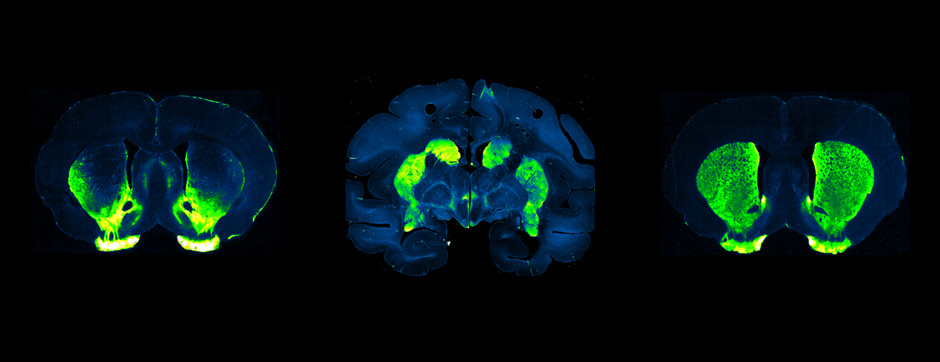
mars 2022 Directeur(s) de thèse : Eric Boué-Grabot Résumé de thèseImplication of neuronal versus glial purinergic receptor P2X4 in chronic neuropathic and inflammatory pain P2X receptors are ATP-gated non-selective cation channels highly permeable to calcium and highly expressed in many tissues. In the central nervous system (CNS), P2X4 is the most widespread P2X receptor and is involved in various pathological states, such as amyotrophic lateral sclerosis, ischemia or chronic pain. It has the particularity to be constitutively internalized and as a result, are found predominantly in intracellular compartments ensuringits low surface expression, in physiological conditions. On the other hand, in pathological condition, P2X4 is overexpressed at the cell-surface, either in neurons and/or glial cells. This is suggesting that neuronal and glial P2X4 receptors may contribute to distinct mechanisms of pathogenesis. P2X4 is playing a key role in the physiological and pathological sensory transduction. Alterations of the purinergic signaling have been shown to be involved in chronic pain syndromes with a pivotal role for microglial P2X4 receptors in neuropathic pain models. Indeed, P2X4 was observed to be increased in the microglia of the dorsal horn of the spinal cord. On the other hand, neuropathic P2X4-depleted mice (P2X4 KO) do not present an increase of their mechanical sensitivity as compared to neuropathic control mice. Unlikely, during inflammatory chronic pain, microglial P2X4 does not seem to be implicated in the pain transduction instead of neuronal P2X4. P2X4 expression was also reported in dorsal root ganglia (DRG) sensory neurons during neuropathic and chronic inflammatory conditions as well as in satellite glial cells that may contribute to both types of pain. Therefore, the neuronal vs. glial implication of P2X4 in neuropathic and inflammatory pain still needs to be unraveled and especially its role at the cell-surface level, as well as sexual dimorphism. In this context, we developed and used novel transgenic mice model in which P2X4 is increased at the cell surface level either in all cells expressing natively P2X4 (P2X4 KI) or in specific cell populations:in neurons (Synapsin-Cre P2X4 KI) or in myeloid cells (CD11b-Cre P2X4 KI mice). First weshowed that higher surface of myeloid P2X4, in Cd11b-Cre P2X4 KI mice, is sufficient to increase mechanical and thermal sensitivities in basal state, in both male and female. This hyperalgesia is also in adequation with a functional increase of the nociceptive transmission recorded in vivo in the dorsal horn projection neurons of the spinal cord of the corresponding
transgenic mouse lines. We then showed that microglial P2X4 was necessary for the development and the maintenance of the chronic neuropathic pain after spared nerve injury (SNI). Regarding inflammatory pain induced by Complete Freund Adjuvant (CFA) in the hind paw in the different transgenic mice, our results indicated that macrophages P2X4 but not neuronal and microglial P2X4 contribute to its development but have no effect in the maintenance of the inflammatory pain.
In conclusion, the development of these novel cell-specific transgenic mouse models and the combination of behavioral, electrophysiological and histological approaches allowed us to unravel the complex implication of P2X4 in neuropathic and inflammatory pain, in both male and female.