Keri-Ann Charles
The pathophysiology of nociceptive abnormalities in the context of Parkinson’s Disease
décembre 2022 Directeur(s) de thèse : Abdelhamid Bennazzouz Résumé de thèsePain is one of the most common causes of disability in public health, not only does it significantly impacts the quality of life of patients both physically and financially, yet it also remains inadequately treated specially in patients with neurological diseases, for example, Parkinson’s disease (PD). PD is the second most common neurodegenerative disorder, present in 1-3% of the world’s population over 60 years of age. It is primarily characterised by its disabling motor symptoms, including but not limited to, tremors, rigidity and bradykinesia. PD also presents a wide range of non-motor symptoms that are usually apparent long before the development of clinical motor signs of the disease. One of the main symptoms is pain, which is experienced by about 80% of PD patients.
Generally, it is admitted that PD is due to the degeneration of dopamine neurons in the substantia nigra pars compacta (SNpc) of the central nervous system. In addition, the pathophysiology of pain in PD also seems to be, at least in part, dependent on this loss of dopamine. The restoration of dopaminergic neurotransmission by L-Dopa has been used successfully for many years in the treatment of motor symptoms. However, its efficacy in the treatment of PD pain forms is not clearly determined. The present study focused on the role of dopamine, especially the dopaminergic A11-spinal cord descending pathway, in pain perception using an animal model of PD.
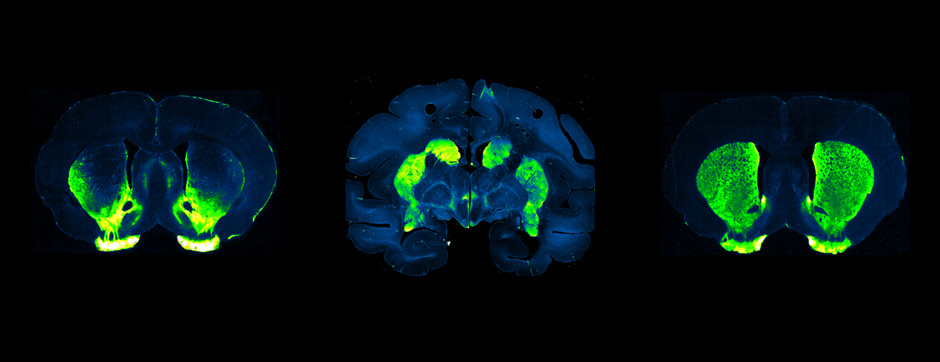
First, we have shown that unilateral lesion of dopamine neurons after the injection of 6-OHDA into the Medial Forebrain Bundle (MFB) decreased paw withdrawal threshold and latency, which corresponds to an increased mechanical allodynia and thermal hyperalgesia, respectively, in hemiparkinsonian rats. In parallel, electrophysiological results showed increased responses of c-fibre’s evoked action potentials of wide dynamic range (WDR) neurons, recorded in the dorsal horn of the spinal cord (DHSC), to electrical nociceptive stimuli of the sciatic nerve. Then, we showed that behavioural and electrophysiological abnormalities in dopamine depleted animals were reversed by intrathecal injections of dopamine agonists with a more pronounced improvement when targeting D2 than D1 dopamine receptors. Finally, we investigated the role of the direct descending pathway from the hypothalamic A11 nucleus to the spinal cord, the only dopaminergic descending projection evidenced as of now. We have shown that partial lesion of A11 neurons significantly reduced nociceptive thresholds.
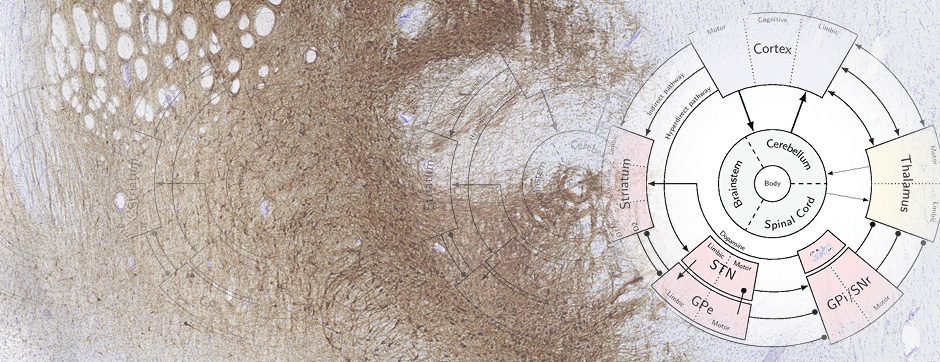
Second, we investigated the role of the subthalamic nucleus (STN) in nociception in normal conditions and in the context of PD. Our electrophysiological results showed that STN neurons presented different responses to the electrical stimulation of the sciatic nerve in a similar way in the two conditions. Furthermore, as chronic deep brain stimulation (DBS) of the STN has been shown to improve pain in the context of PD, we have investigated the influence of STN DBS on nociceptive integration in the spinal cord. We have shown that STN DBS induced a decrease in the number of spike C of WDR neurons demonstrating a normalization of nociceptive integration in the DHSC. This effect was reversed by the microinjection of lidocaine in the raphe magnus nucleus.
Results of these studies show first, that dopamine projections to the spinal cord are involved in pain hypersensitivity in our rat model of PD, highlighting the primary role of the hypothalamic nucleus A11 in the pathophysiology of pain in PD. Second our results support also the idea that the STN, which is known to play an important role in the pathophysiology of PD motor disabilities, is also involved in the nociceptive abnormalities associated to PD.
Our study provides new insights into the pathophysiology of pain in PD and opens the way to new therapeutic approaches targeting this disabling non-motor symptom of the disease.